Overview
What are actinic keratoses?
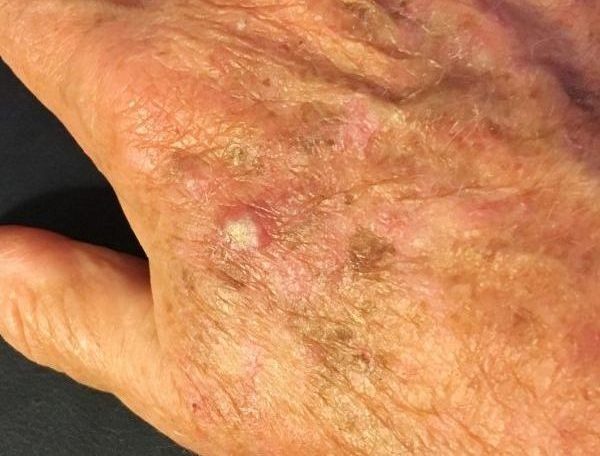
Actinic keratoses are dry, rough, scaly patches or small bumps that appear on areas of the skin that have been damaged by repeated or prolonged exposure to UV radiation. These patches may be skin-coloured, pink, red or brown and often feel like sandpaper when touched.
Although they are not usually serious, actinic keratoses are considered precancerous because they reflect damage to skin cells and have the potential to progress to squamous cell carcinoma over time. Early identification and monitoring are key.
Where do actinic keratoses commonly appear?
These lesions most often develop on sun-exposed parts of the body, including:
- The face, ears and scalp (especially in people with thinning or no hair)
- The backs of the hands and forearms
- The neck and chest
- Lips and lip borders (a form known as actinic cheilitis)
Symptoms and Causes
Recognising the signs of actinic keratoses
Actinic keratoses may have one or more of the following features:
- Rough, dry or scaly patches of skin
- Flat or slightly raised lesions that feel sandpapery
- Skin-toned, pink, red or brown discolouration
- Itching, tenderness, burning or discomfort in some cases
- Occasional bleeding or crusting, especially if irritated
Many actinic keratoses are painless and may go unnoticed until closely examined. Multiple lesions often occur in the same area.
What causes actinic keratoses?
Actinic keratoses develop as a result of cumulative UV radiation damage to the skin’s cells, most commonly from years of sun exposure and, in some cases, tanning bed use. UV rays damage the DNA in skin cells, leading to abnormal growth and changes in the outer layer of skin.
Who is at increased risk?
Anyone can develop actinic keratoses, but the risk is higher in people who:
- Have fair skin, light eyes or hair and a tendency to burn in the sun
- Are aged over 40, due to cumulative sun exposure
- Spend a lot of time outdoors or work in the sun
- Live in sunny climates or closer to the equator
- Have a weakened immune system, such as after organ transplantation or due to medical therapy
Diagnosis and Tests
How are actinic keratoses diagnosed?
Diagnosis is usually made by a GP or dermatologist based on the appearance, texture and location of the lesions during a clinical skin examination. Actinic keratoses often have a characteristic rough, sandpaper-like feel that makes them easier to identify by touch than by sight alone.
A dermatoscope, a hand-held magnifying tool, may be used to view the skin more closely.
When is a biopsy needed?
If a lesion looks unusual, grows quickly, bleeds, crusts, or has features suggestive of skin cancer, a small sample of skin (biopsy) may be taken and examined in a laboratory to rule out squamous cell carcinoma or other skin cancers.
Management and Treatment
How are actinic keratoses treated?
The aim of treatment is to remove the abnormal skin cells and reduce the risk of progression to skin cancer. The choice of treatment depends on the number, size and site of the lesions, as well as patient preference and skin type.
Common treatment options include:
- Cryotherapy: Freezing the lesion with liquid nitrogen to destroy abnormal cells.
- Topical treatments: Prescription creams or gels, such as 5-fluorouracil, imiquimod or diclofenac, applied to the skin over several weeks.
- Photodynamic therapy (PDT): A light-activated treatment that targets abnormal cells after applying a photosensitising agent.
- Curettage and cautery: Scraping and burning off the lesion when necessary.
- Laser therapy: Using focused light to remove damaged skin.
- Surgical excision: Removing the lesion under local anaesthetic, typically for larger or suspicious areas.
Some treatments may cause redness, peeling, irritation or tenderness as part of the healing process. Your clinician will discuss what to expect and how to care for your skin during treatment.
Outlook/Prognosis
What happens over time?
Actinic keratoses do not usually go away on their own and may persist or recur without treatment. Treatment often clears lesions and can reduce the risk of progression to skin cancer, but there is a possibility that new lesions may develop over time, particularly in areas exposed to sunlight.
Can actinic keratoses progress to skin cancer?
Actinic keratoses are considered precancerous. While many do not progress, some can evolve into squamous cell carcinoma if left untreated or if sun damage continues. This is why monitoring and appropriate management are important.
Prevention
Can actinic keratoses progress to skin cancer?
It may not be possible to prevent all actinic keratoses, but reducing UV exposure and protecting the skin can significantly lower the risk.
Helpful measures include:
- Limiting time in the sun, especially between 10 a.m. and 4 p.m.
- Wearing a broad-spectrum sunscreen with SPF 30 or higher every day
- Wearing sun-protective clothing, wide-brimmed hats and sunglasses
- Avoiding tanning beds and artificial UV sources
- Regularly checking the skin for new or changing patches and seeking early assessment
When to seek medical advice
You should see a GP or dermatologist if you notice:
- A rough, scaly patch that persists or grows
- Bleeding, crusting, pain or tenderness
- A lesion that changes quickly in appearance
- New patches on sun-exposed areas
- Concern about appearance or discomfort
Prompt assessment can help rule out skin cancer and ensure timely treatment.