Noticing white spots or pale patches on your skin can feel worrying, especially if they appear suddenly or begin to spread. In many cases, these changes are harmless and simply reflect minor changes in skin pigmentation. However, white spots can sometimes be linked to common skin conditions such as fungal infections, eczema, or autoimmune disorders like vitiligo.
Noticeable white patches can appear on the skin for many reasons. Some are harmless signs of ageing or mild skin changes, while others result from treatable conditions. Often white spots form when normal skin pigment (melanin) is lost or when keratin (dead skin cells) accumulates under the skin.
For example, vitiligo is a long-term autoimmune condition where patches of skin turn milky-white due to destruction of pigment cells.
Although white spots may look alarming, they usually aren’t serious. However, it is still wise to have new or changing patches checked by a GP or dermatologist.
Why white spots appear on the skin
Skin colour is determined by melanin, which is produced by specialised cells called melanocytes located in the outer layer of the skin. These cells give skin its natural colour and help protect the body from ultraviolet radiation.
White spots can appear when melanin production decreases, when pigment-producing cells are damaged, or when other processes interfere with normal pigmentation. In some cases inflammation, infection, or injury temporarily disrupts pigment production. In other situations pigment-producing cells may be lost completely.
Sometimes white bumps develop because keratin becomes trapped beneath the skin’s surface. This is what happens in conditions such as milia.
The size, shape, and location of white spots can often help identify the underlying cause.
Common causes of white spots on skin
White spots can develop for several reasons. The most common causes include sun-related pigment loss, fungal infections, mild eczema, autoimmune pigment disorders, and hypopigmentation that occurs after skin inflammation.
Because several different conditions can cause white patches or pale spots, the table below summarises the most common causes and their key features.
| Condition | Typical Appearance | Common Locations | Key Features | Treatment |
|---|---|---|---|---|
| Idiopathic guttate hypomelanosis | Small round white spots | Forearms, shins, shoulders | Linked to ageing and sun exposure | Usually no treatment required; sun protection recommended |
| Tinea versicolor | Light or discoloured patches with mild scaling | Chest, back, neck, upper arms | Caused by yeast overgrowth; patches do not tan normally | Antifungal creams or medicated shampoos |
| Pityriasis alba | Pale patches with soft edges | Face, cheeks, upper arms | Mild eczema common in children and teens | Moisturising creams; mild steroid cream if needed |
| Vitiligo | Clearly defined bright white patches | Face, hands, elbows, knees | Autoimmune condition affecting melanocytes | Prescription creams, phototherapy, sun protection |
| Milia | Tiny white bumps | Around eyes, cheeks, forehead | Keratin trapped beneath skin surface | Usually resolves naturally; dermatologist removal if needed |
| Post-inflammatory hypopigmentation | Lighter patches after skin irritation | Anywhere previous rash or injury occurred | Follows eczema, burns, or infections | Often resolves naturally as skin heals |
Idiopathic guttate hypomelanosis

One of the most common causes of small white spots is idiopathic guttate hypomelanosis, sometimes described as “sunspots in reverse”.
These tiny porcelain-white spots typically appear on sun-exposed areas such as the shins and forearms. They occur frequently in older fair-skinned people and are believed to result from many years of sun exposure gradually reducing melanin in the skin.
The spots usually have smooth, well-defined edges and are harmless. They are considered a cosmetic change rather than a medical condition.
There is currently no proven treatment to remove these spots. Many people simply use sunscreen or cosmetic cover-up if they are concerned about their appearance.
Tinea versicolor
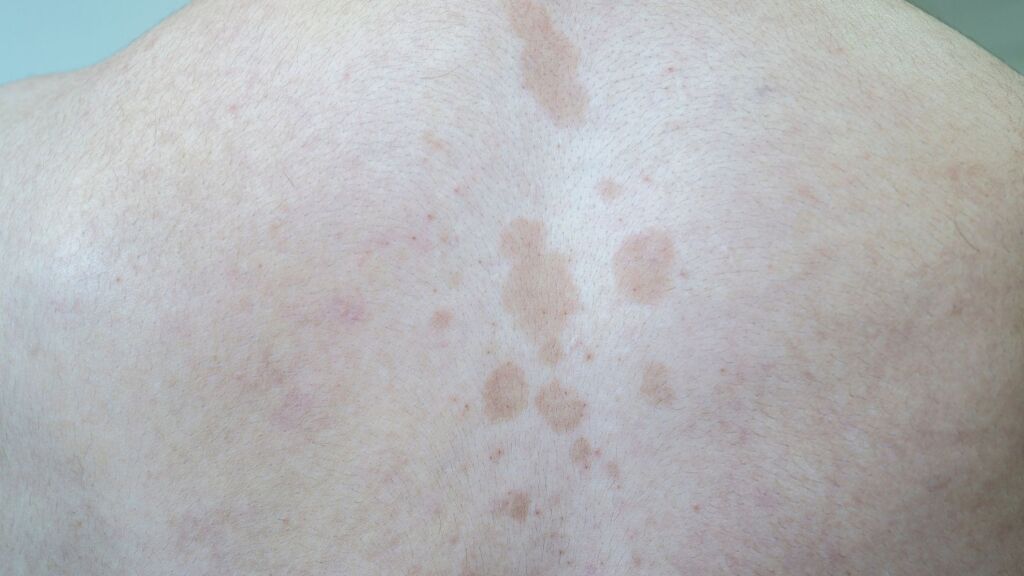
Tinea versicolor, also known as pityriasis versicolor, is a common fungal infection of the skin.
It causes flat, round patches that can appear lighter or darker than the surrounding skin. On lighter skin tones the spots may look pinkish or pale, while on darker skin tones they may appear light or yellow-brown.
The rash most often develops on:
- chest
- back
- upper arms
- neck
These patches may feel slightly scaly and can sometimes cause mild itching.
A key feature of tinea versicolor is that the affected areas do not tan normally, which means the spots often become more noticeable after sun exposure.
Because the condition is caused by yeast, it can recur, particularly in warm or humid weather.
Pityriasis alba
Pityriasis alba is a mild form of eczema commonly seen in children and teenagers.
The condition often begins as a slightly red or flaky rash which gradually fades, leaving round or oval pale patches on the skin. These patches frequently appear on the cheeks but may also develop on the neck or upper arms.
The edges of pityriasis alba patches tend to be softer and less clearly defined than those seen in vitiligo.
Pityriasis alba is usually self-limiting, meaning the patches gradually fade over time. Gentle moisturising and mild steroid creams may help if there is dryness or irritation.
Vitiligo

Vitiligo is an autoimmune condition in which melanocytes, the cells responsible for producing skin pigment, are destroyed.
This results in larger white patches of skin that often appear symmetrically, such as on both hands or both sides of the face. Many people first notice vitiligo before the age of twenty.
Vitiligo causes clearly defined milky-white areas of skin. Although the condition is not contagious, it can sometimes be distressing due to its visible nature.
Milia
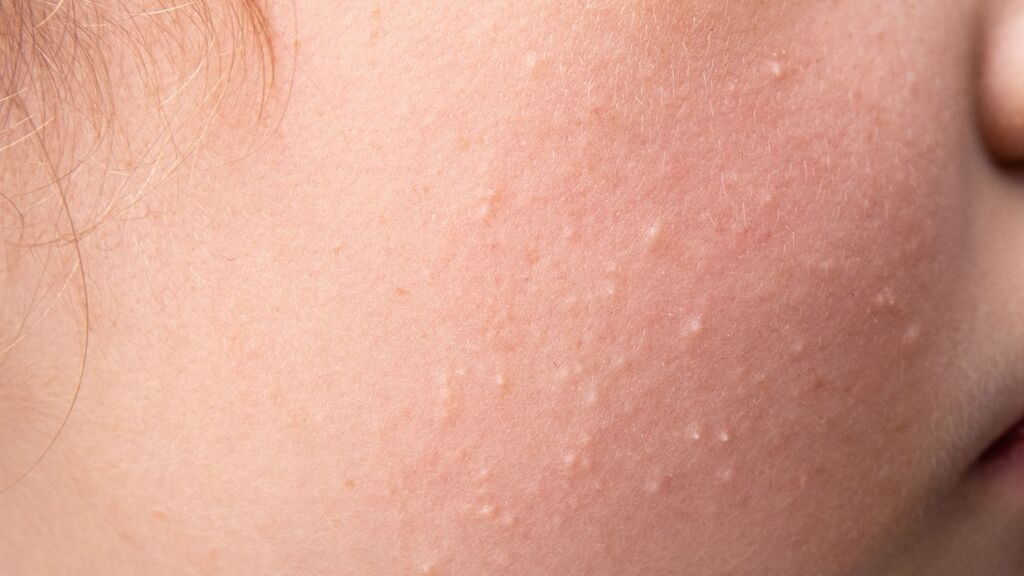
Milia are tiny, firm white bumps commonly found on the face, particularly around the eyes, cheeks or forehead. They can also appear on the scalp or nose of newborn babies, where they are sometimes referred to as “milk spots.”
These bumps form when keratin becomes trapped beneath the skin’s surface, creating small cysts just under the skin.
Milia can occur in both babies and adults. In newborns they are very common and usually clear within a few weeks without treatment. In adults they may develop after skin irritation, sun damage or the use of heavy skincare products.
Milia are harmless and often disappear naturally over time. If removal is desired for cosmetic reasons, a dermatologist can safely remove them during a simple in-clinic procedure.
Post-inflammatory hypopigmentation
White spots can also appear after the skin heals from inflammation or injury. This is known as post-inflammatory hypopigmentation.
It may occur after skin conditions such as eczema, burns, psoriasis, infections, or allergic reactions. During healing, the skin may temporarily lose pigment in affected areas.
These patches often have irregular borders and may gradually fade as the skin regenerates.
Other less common causes
Although less common, some conditions can also cause pale patches of skin.
Examples include:
- congenital birthmarks such as nevus depigmentosus
- genetic mosaicism
- lichen sclerosus, which may cause white patches on genital or chest skin
However, these causes account for a small proportion of cases compared with the conditions described above.
Risk factors for white spots
Certain factors may increase the likelihood of developing white spots on the skin, including:
- long-term sun exposure
- genetic predisposition
- autoimmune conditions
- oily skin that encourages fungal growth
- previous skin inflammation or injury
Understanding these risk factors can help people recognise potential triggers and protect their skin health.
How doctors diagnose white spots
Doctors usually diagnose white spots through a visual examination of the skin. The pattern and location of the patches often provide important clues about the underlying condition.
In some cases additional tests may be used, including:
- Wood’s lamp examination, which uses ultraviolet light to highlight pigment changes
- skin scraping tests to check for fungal infection
- skin biopsy, rarely used if the diagnosis is unclear
These tests help ensure the correct condition is identified so appropriate treatment can be recommended.
When to See a Doctor
Most white spots are harmless and do not require treatment. However, it is sensible to seek medical advice if the patches change or cause concern.
A healthcare professional should evaluate spots that spread rapidly, increase in number, become itchy or painful, or change in texture. Persistent patches that do not improve over time may also benefit from medical assessment.
Treatment Options
Treatment depends entirely on the underlying cause of the pigmentation change.
Tinea versicolor is usually treated with antifungal shampoos or creams containing medications such as ketoconazole or selenium sulphide. These treatments eliminate the yeast responsible for the infection, although the skin colour may take several weeks or months to return to normal.
For conditions such as pityriasis alba or post-inflammatory hypopigmentation, gentle skin care and regular moisturising are often sufficient. If inflammation is present, a doctor may recommend a mild topical corticosteroid cream.
Vitiligo treatments aim to restore pigment or slow the spread of patches. These may include prescription creams or light-based therapies such as narrowband UVB phototherapy. Because depigmented skin burns easily, regular use of broad-spectrum sunscreen is important.
Can White Spots Be Prevented?
Not all white spots can be prevented, but maintaining healthy skin habits can reduce the risk of certain pigment changes.
Protecting the skin from excessive sun exposure is particularly important. Regular use of sunscreen helps prevent sun damage and may reduce the likelihood of developing white sunspots.
Keeping the skin moisturised, avoiding harsh skincare products, and treating fungal infections early can also help maintain a healthy skin barrier.
Frequently asked questions
Are white spots on skin dangerous?
Most white spots are harmless and related to pigmentation changes or mild skin conditions. However, it is advisable to seek medical advice if the patches spread, change, or cause symptoms.
Why do white spots become more visible after sun exposure?
In conditions such as tinea versicolor or vitiligo, the affected areas cannot tan normally. When surrounding skin darkens in the sun, the contrast makes the lighter patches more noticeable.
Can white spots disappear on their own?
Some causes, such as pityriasis alba or post-inflammatory hypopigmentation, often improve naturally over time. Others, such as vitiligo or idiopathic guttate hypomelanosis, may persist without treatment.
Can home remedies treat white spots?
While some natural remedies are suggested online, medical treatments are generally more reliable. Antifungal creams or medicated shampoos are the most effective treatments for fungal infections like tinea versicolor.
Conclusion
White spots on the skin are usually caused by changes in skin pigmentation, fungal infections, mild eczema, or autoimmune conditions such as vitiligo. In most cases they are harmless and manageable with proper care.
If you notice white patches that spread, persist, or cause concern, consulting a healthcare professional can help identify the underlying cause and determine whether treatment is needed.

Concerned about white spots or skin changes? Book a free skin assessment and get expert advice from our dermatology specialists.
- Medical Disclaimer:
This article is for informational purposes only and does not replace professional medical advice. If you are concerned about changes in your skin, consult a qualified healthcare professional.






 WHATSAPP
WHATSAPP