Overview
What is skin cancer?
Skin cancer develops when damage to the DNA of skin cells disrupts their normal growth cycle. Healthy skin cells grow, divide and are replaced in a controlled way. When DNA damage is not repaired, abnormal cells may continue to divide and accumulate, forming a malignant tumour. These cancerous cells can invade nearby tissue and, in some cases, spread to other parts of the body.
Many skin cancers are slow growing and highly treatable when detected early, but some types can spread to other parts of the body and become serious if diagnosis or treatment is delayed.
What causes skin cancer?
The most common cause of skin cancer is exposure to ultraviolet (UV) radiation. UV radiation damages the DNA in skin cells over time, increasing the risk of abnormal cell growth. Sources of UV radiation include:
- Natural sunlight
- Sunbeds and tanning lamps
Other factors that may contribute include genetic susceptibility, a weakened immune system, increasing age and a personal history of skin cancer.
How common is skin cancer?
Skin cancer is one of the most common cancers worldwide. Non-melanoma skin cancers, such as basal cell carcinoma and squamous cell carcinoma, account for the majority of cases. Melanoma is less common but is responsible for a higher proportion of skin-cancer-related deaths because it is more likely to spread if not detected early.
Who is at risk?
Skin cancer can occur in anyone, but risk is higher in people who:
- Have frequent or intense exposure to UV radiation
- Have fair skin that burns easily
- Have light hair or light-coloured eyes
- Have many moles or atypical moles
- Have a personal or family history of skin cancer
- Use tanning beds
- Have a weakened immune system
People with darker skin tones can also develop skin cancer, although it may be less common and sometimes diagnosed later.
Where on the body does skin cancer usually appear?
Skin cancer most often develops on areas exposed to the sun, including the face, scalp, ears, neck, arms and hands. It can also occur on areas that receive little sun exposure, such as the palms, soles of the feet, nails and genital skin, particularly in melanoma.
Types of skin cancer
The main types include:
- Basal cell carcinoma (BCC):
The most common type. BCC usually grows slowly and rarely spreads to other parts of the body, but it can damage surrounding tissue if left untreated. - Squamous cell carcinoma (SCC):
Less common than BCC but more likely to grow deeper into the skin and spread if not treated promptly. - Melanoma:
The least common but most serious type. Melanoma develops from pigment-producing cells and can spread to lymph nodes and other organs if not detected early.
Rarer forms include Merkel cell carcinoma and other uncommon skin tumours.
Symptoms and Causes
What are the symptoms of skin cancer?
Skin cancer does not always cause pain or discomfort. Possible signs include:
- A new spot, lump or growth on the skin
- A sore that does not heal
- A scaly, crusted or bleeding area
- A mole that changes in size, shape or colour
Changes may develop slowly over time and may not cause symptoms initially.
What skin changes should raise concern?
Seek assessment for skin changes such as:
- Rapid growth
- Irregular or poorly defined borders
- Changes in colour or multiple colours in one lesion
- Persistent itching, tenderness or bleeding
- A lesion that looks different from others on the body
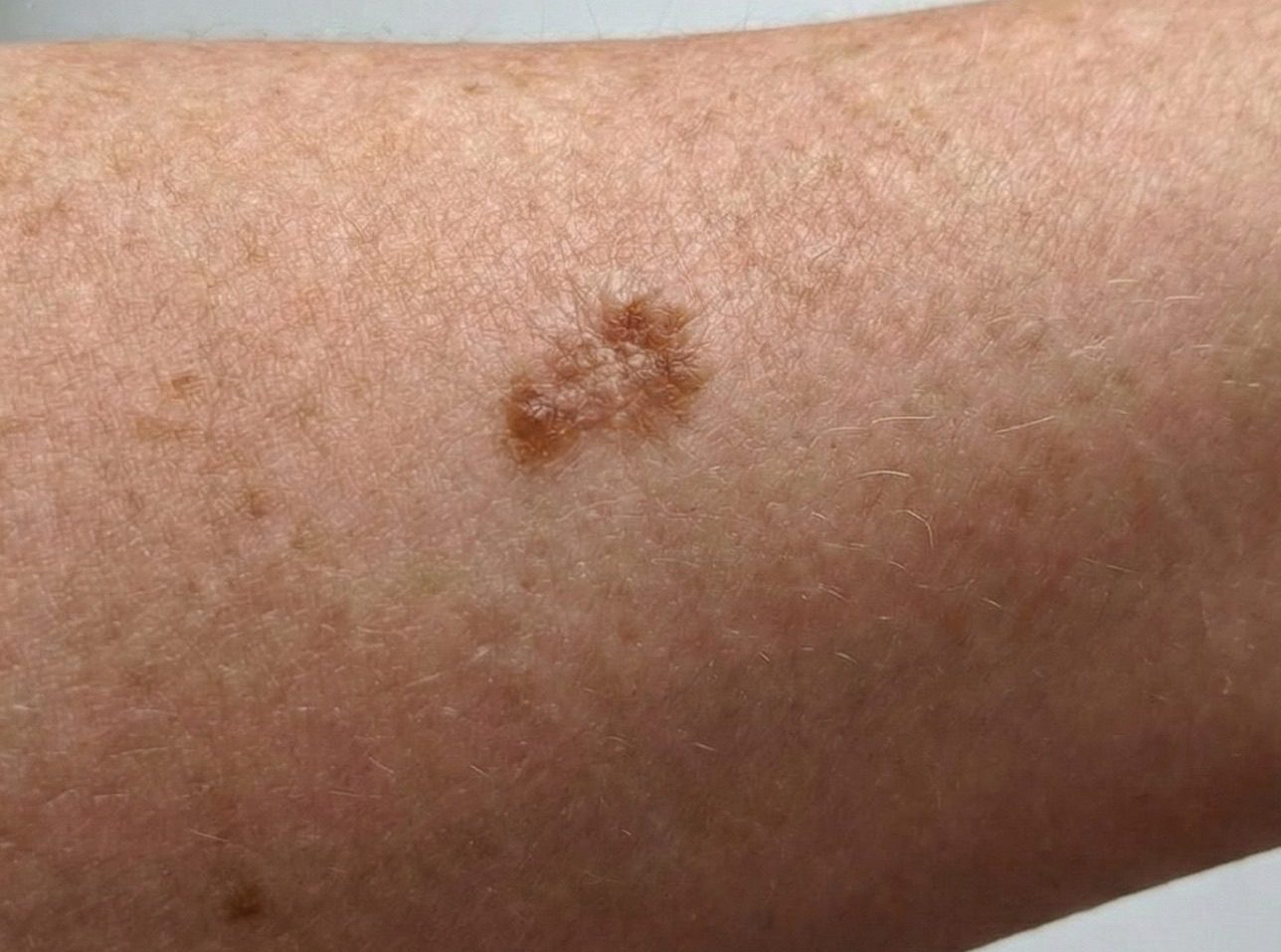
What does melanoma look like?
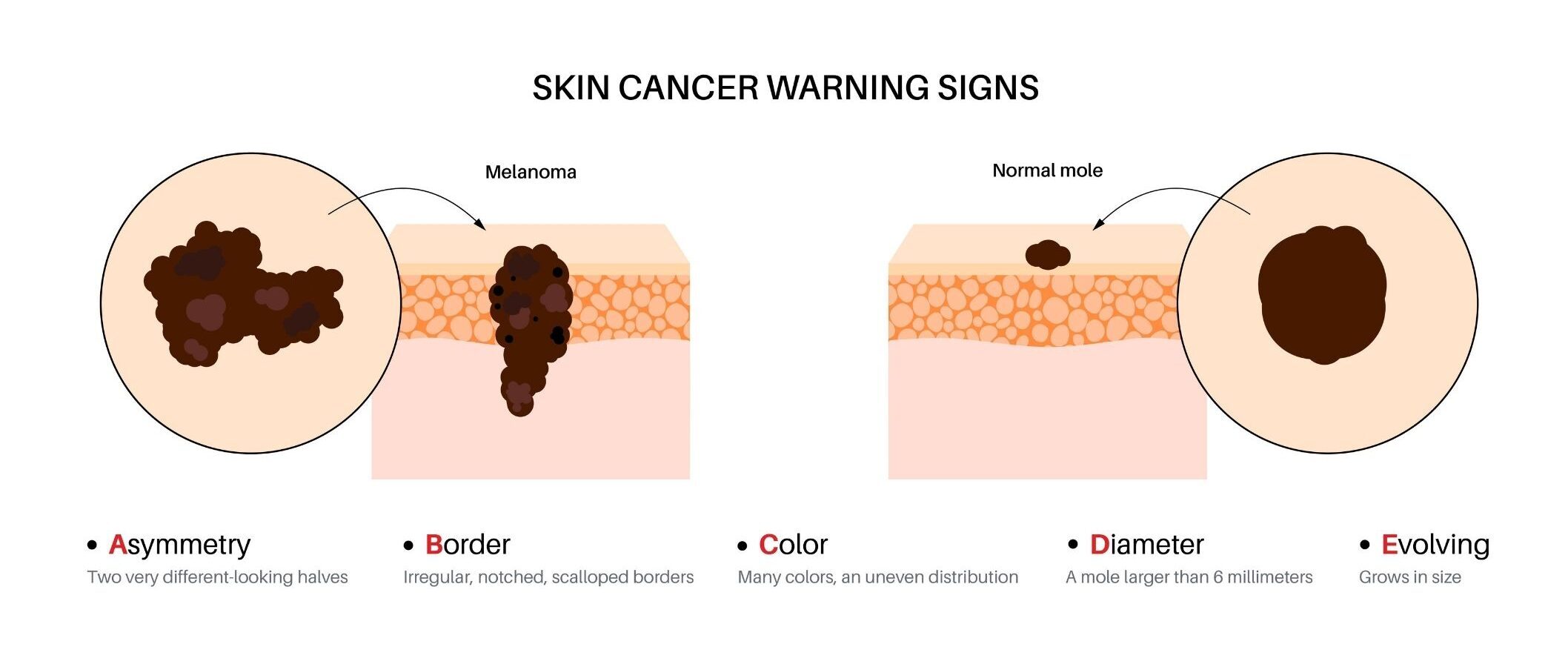
Melanoma often appears as a new mole or a change in an existing mole. The ABCDE guide can help identify concerning features:
- Asymmetry
- Border irregularity
- Colour variation
- Diameter increasing
- Evolving in size, shape or colour
What does non-melanoma skin cancer look like?
- Basal cell carcinoma: Pearly or shiny bumps, pink patches, or sores that heal and then return
- Squamous cell carcinoma: Firm nodules, rough scaly patches, or ulcers that may crust or bleed
Diagnosis and Tests
How is skin cancer diagnosed?
Specialists combine visual and clinical assessment with laboratory and imaging tests to confirm the type and extent of skin cancer.
Key diagnostic steps:
- Full skin examination: Inspection of the entire body, including scalp, palms, soles, and between toes, to identify suspicious lesions.
- Dermoscopy: Magnified evaluation of moles or lesions to identify early signs of malignancy.
- Biopsy: A small tissue sample is removed to confirm the type, depth, and severity of the cancer.
- Imaging: Ultrasound, CT, or MRI may be used for deeper lesions or to check lymph nodes in advanced cases.
- Histopathology: Laboratory examination of biopsy samples ensures an accurate diagnosis and informs treatment planning.
Accurate diagnosis is essential for effective treatment, prognosis, and patient confidence.
Are imaging tests ever needed?
Imaging tests such as ultrasound, CT or MRI may be used if there is concern that the cancer has spread beyond the skin.
When should you see a GP or dermatologist?
You should seek medical advice if:
- Acne is moderate to severe
- Acne persists despite over-the-counter treatments
- Spots are painful or widespread
- Scarring is occurring
- There is significant emotional or mental health impact
A dermatologist can offer specialist care and advanced treatments.
Management and Treatment
How is skin cancer treated?
Treatment depends on the type, location, size, and stage of the cancer, as well as the patient’s overall health and preferences.
Treatment options
Outlook/Prognosis
The prognosis for skin cancer varies depending on the type and how early it is detected. Basal cell carcinoma (BCC) and squamous cell carcinoma (SCC) are generally highly treatable, and early intervention usually carries minimal risk of complications or spread. Melanoma, while less common, can be more serious; outcomes are excellent when detected early, but delayed treatment increases the risk of metastasis to other organs. Regular follow-up and long-term skin monitoring are essential to ensure early detection of any new or recurring lesions and to maintain overall skin health.
Can skin cancer come back after treatment?
Yes. People who have had skin cancer have a higher risk of recurrence or developing a new skin cancer, which is why follow-up and regular skin checks are important.
Prevention
Can skin cancer be prevented?
While not all skin cancers can be prevented, the following measures reduce risk:
- Use broad-spectrum sunscreen and protective clothing
- Avoid tanning beds and limit sun exposure
- Regular self-examination of the skin for new or changing lesions
- Attend routine dermatology assessments, particularly for high-risk individuals
- Seek prompt evaluation of any suspicious lesions
How often should you check your skin?
Regular self-examination helps identify changes early. Any persistent or changing lesion should be discussed with a healthcare professional.