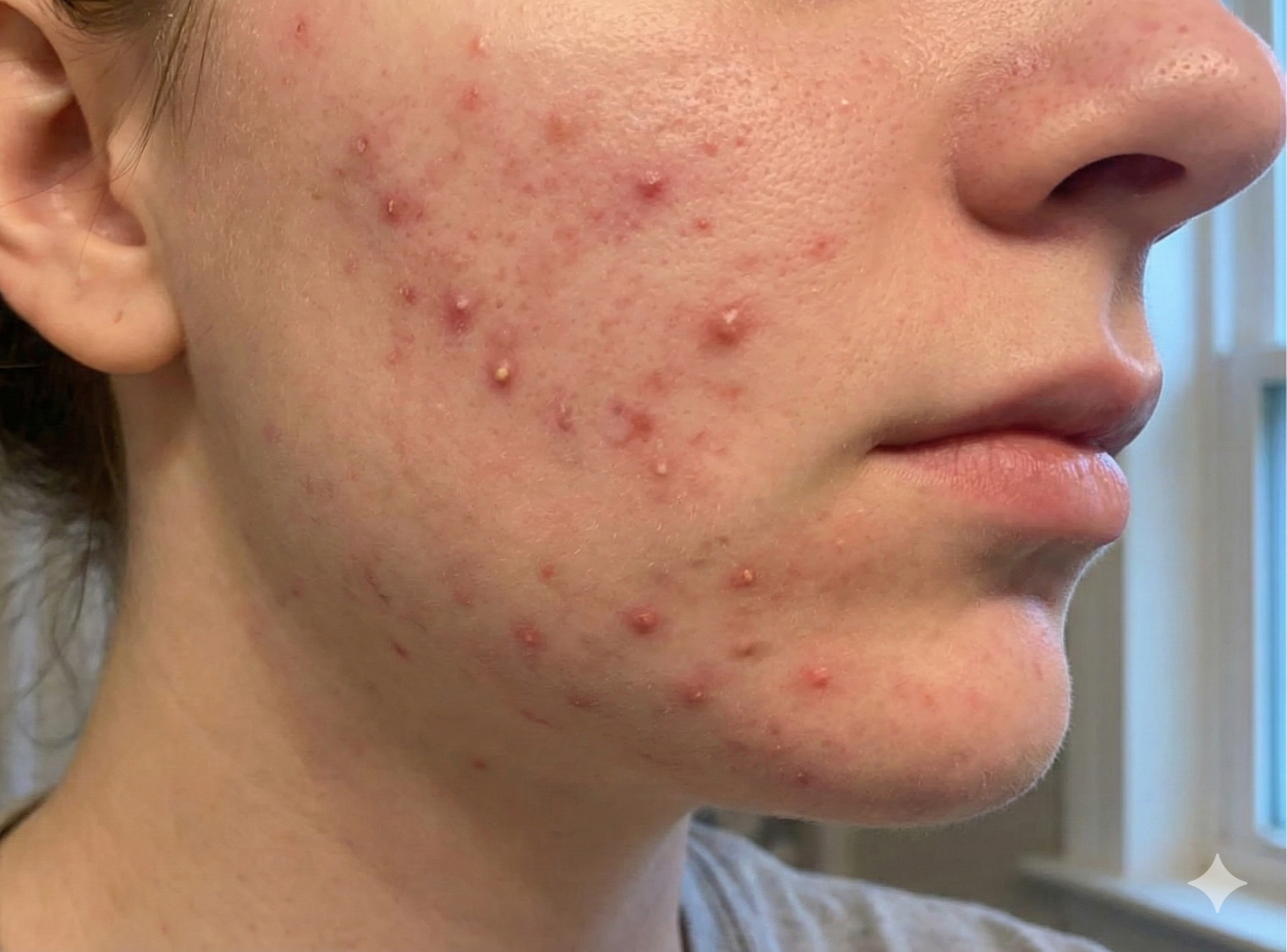
Overview
What is acne?
Acne, also known as acne vulgaris, occurs when the sebaceous glands attached to hair follicles become overactive. These glands produce sebum, an oily substance that helps protect the skin. When too much sebum is produced, it can combine with dead skin cells to block the follicle opening.
Within these blocked pores, naturally occurring skin bacteria (Cutibacterium acnes) can multiply. This process triggers inflammation, leading to the formation of visible acne lesions such as blackheads, pimples and deeper, painful lumps.
Who gets acne?
Most people experience acne at some point. It is especially common during adolescence due to hormonal changes, but many adults continue to have acne into their 20s, 30s and beyond. Adult acne is more common in women and often linked to hormonal fluctuations. Mild acne-like spots, often referred to as baby acne, can also occur in newborns and infants, but this form usually resolves on its own and is different from adolescent or adult acne.
How common is acne?
Acne is one of the most common skin conditions in the UK and worldwide. The vast majority of teenagers experience acne at some stage, and many adults continue to have breakouts beyond their teen years. Around 85% of people aged 12–24 have acne to some degree, and a notable number of adults also experience ongoing spots past their twenties.
Does acne run in families?
Genetics plays a significant role in acne susceptibility. Having a family history of acne increases the likelihood of developing the condition, suggesting inherited differences in sebum production and skin response.
Where does acne usually appear?
Acne typically appears in areas with more oil glands — most often on the face, chest, upper back and shoulders. These are the parts of the skin most prone to clogged follicles and inflammation.
Is acne more common in women or men?
During adolescence, acne can be more severe in males. In adulthood, acne is frequently reported in women, often associated with hormonal changes such as menstrual cycles, pregnancy or menopause.
What are the different types of acne?
Acne can present as different lesion types, including:
- Blackheads: Open blocked pores with a dark surface
- Whiteheads: Closed blocked pores under the skin
- Papules: Small, red, tender bumps
- Pustules: Spots containing visible pus
- Nodules: Large, firm lumps deep below the skin
- Cysts: Deep, pus-filled painful lesions with a higher risk of scarring
When acne mainly consists of blackheads and whiteheads, it is referred to as comedonal acne. When inflammation is present, including papules and pustules, it is described as inflammatory acne. More severe forms include nodular acne and cystic acne, both of which develop deeper within the skin and are more likely to result in permanent scarring if not treated appropriately.
Hormonal acne commonly affects the lower face, jawline and chin and may flare in response to hormonal fluctuations. All forms of acne develop from blocked pores, but inflammatory and deeper lesions carry a greater risk of pain, pigmentation changes and scarring if left untreated.
Note: Some conditions, such as fungal acne (Malassezia folliculitis), can resemble acne but are caused by yeast rather than blocked pores and require a different treatment approach.
Symptoms and Causes
What are the symptoms of acne?
Common acne symptoms include:
- Blackheads and whiteheads
- Red, tender bumps (papules, pustules)
- Larger, painful lumps under the skin (nodules, cysts)
- Red or dark marks after spots heal
- Oily or shiny skin
Severity varies from occasional mild spots to widespread, inflamed lesions that can be painful and long-lasting.
What causes acne?
Acne occurs when hair follicles become clogged with excess oil, dead skin cells and bacteria. Hormonal changes, particularly increased androgen levels, stimulate oil production and worsen blockage and inflammation. Genetics also influence susceptibility.
Does stress make acne worse?
Stress does not directly cause acne, but it can aggravate existing acne by increasing inflammation and hormonal activity that stimulates oil production.
Do hormones affect acne?
Hormones, especially androgens such as testosterone, increase sebum production and are a key factor in acne development. Hormonal fluctuations during puberty, menstruation and pregnancy are common triggers.
Triggers and risk factors
Common triggers and risk factors that can worsen acne include:
- Hormonal changes (puberty, menstrual cycle, pregnancy or menopause)
- Certain medications (e.g. corticosteroids, testosterone supplements)
- Oily or comedogenic skincare products
- Friction or pressure on skin (e.g. helmets, backpack straps)
- Stress
- Smoking and certain lifestyle factors
- Picking or squeezing spots, which can worsen inflammation and risk scarring
There is no strong evidence that poor hygiene causes acne; excessive washing may irritate the skin and make symptoms worse. While diet (e.g. high glycaemic foods or dairy) has been linked to acne in some studies, the evidence is not definitive and varies between individuals.
Diagnosis and Tests
How is acne diagnosed?
Acne is diagnosed clinically by a GP or dermatologist based on the appearance, number and type of lesions. A clinician may also ask about onset, triggers, sleep, diet and medication history. Hormonal tests may be considered if acne appears suddenly in adulthood or alongside other symptoms like irregular periods.
Is acne a sign of an underlying condition?
Acne is typically a common skin issue. However, when acne starts suddenly in adulthood or occurs alongside irregular periods or excess hair growth, underlying hormonal conditions such as polycystic ovary syndrome (PCOS) may be considered.
When should you see a GP or dermatologist?
You should seek medical advice if:
- Acne is moderate to severe
- Acne persists despite over-the-counter treatments
- Spots are painful or widespread
- Scarring is occurring
- There is significant emotional or mental health impact
A dermatologist can offer specialist care and advanced acne treatments.
Management and Treatment
How is acne treated?
Treatment depends on acne severity and individual factors. It aims to reduce sebum production, prevent blocked pores, limit bacterial growth and control inflammation. Many treatments take several weeks to months to show benefit.
What treatments are used for different severities of acne?
- Mild acne: Topical treatments such as benzoyl peroxide, azelaic acid or retinoids
- Moderate acne: Combination topical treatments and short courses of antibiotics
- Severe acne: Specialist acne treatments such as laser therapy, oral isotretinoin or hormonal therapies
Treatment choice depends on severity, skin type and individual response.
Can acne come back after treatment stops?
Yes. Acne can recur, especially if underlying triggers such as hormonal fluctuations persist. Maintenance treatment may help keep acne under control long-term.
Outlook/Prognosis
What to expect over time with acne?
Acne often improves with age, especially as hormone levels stabilise, but it can persist into adulthood for some people. Inflammatory acne, particularly cysts and nodules, has a higher risk of permanent acne scarring, especially if spots are picked or squeezed. Persistent acne may affect mental wellbeing, particularly when it is long-lasting or severe.
Can acne cause permanent scarring?
Yes. Acne can cause permanent scarring, particularly when inflammatory lesions (nodules and cysts) damage deeper skin layers. Picking or squeezing spots increases scar risk. Early, effective treatment reduces this risk.
Prevention
While acne cannot always be prevented, flare-ups may be reduced by:
- Washing affected areas gently once or twice a day with a mild, non-abrasive cleanser
- Using oil-free, non-comedogenic skincare and makeup
- Avoiding harsh scrubs and over-cleansing
- Avoiding picking or squeezing spots
- Protecting skin from prolonged sun exposure
Lifestyle habits such as managing stress and maintaining a balanced diet may also support overall skin health.
When to seek medical advice
See a GP or dermatologist if:
- Acne is moderate or severe
- Over-the-counter treatments have not worked
- Acne is causing scarring, pain, widespread inflammation or significant emotional distress
- There are sudden changes in the pattern or severity of acne
Early assessment can help guide appropriate treatment and reduce the risk of complications such as scarring.